The Battle Beneath Your Skin: How Keratinized and Nonkeratinized Stratified Squamous Epithelium Safeguard Your Body
The Battle Beneath Your Skin: How Keratinized and Nonkeratinized Stratified Squamous Epithelium Safeguard Your Body
Beneath the visible surface of human skin lies an intricate, dynamic defense system—unseen yet relentless. Composed of two primary architectural layers—keratinized and nonkeratinized stratified squamous epithelium—these tissues form the body’s frontline protection against mechanical stress, pathogens, and environmental wear. This complex biological barrier, honed by millions of years of evolution, serves not merely as a static shield but as a responsive, adaptive interface that maintains integrity across diverse physiological demands.
From the friction-prone palms to the moist mucosal linings, the strategic placement of these epithelial subtypes reveals an elegant balance between protection and functionality.
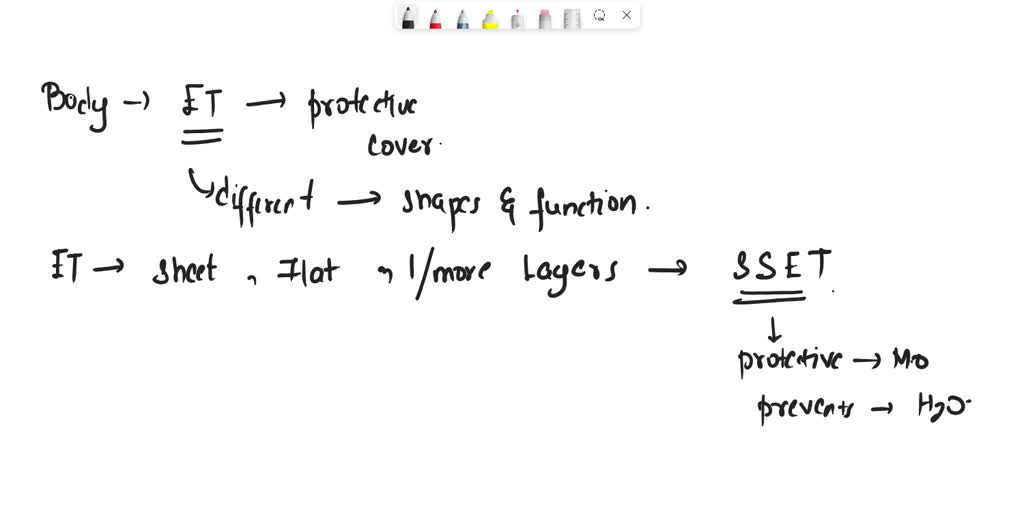
Keratinized stratified squamous epithelium stands at the forefront of tough, external defense. Composed of tightly packed, flattened cells rich in keratin—a tough, fibrous protein formed during differentiation—this tissue forms a waterproof, abrasion-resistant layer.
Characterized by multiple layers of estrangulated cells, it acts as an impermeable barrier against abrasion, chemical irritants, and microbial invaders. The outermost stratum corneum, densely packed with keratin and lipids, effectively prevents water loss and blocks entry points for pathogens, minimizing infection risks. “This layer evolves in response to mechanical stress,” explains dermatologist Dr.
Elena Torres, “acting as both armor and mediator—protecting while allowing controlled interaction with the external world.” Commonly found in the skin’s handpads, stratum corneum is the body’s first line against cuts, scrapes, and environmental assaults, enduring constant friction with minimal degradation.
Nonkeratinized Stratified Squamous Epithelium: Soft yet Resilient
In contrast, nonkeratinized stratified squamous epithelium thrives in mucosal and internal environments where flexibility and moisture retention are paramount. Located in hidden yet vital regions—such as the lining of the mouth, esophagus, and vagina—this tissue maintains a living, moist surface lined with living cells continuously renewed through mitosis.Unlike its keratinized counterpart, this epithelium lacks significant keratin deposition, preserving elasticity and permitting normal physiological functions like swallowing and respiration. Though less robust in mechanical resistance, its intimate contact with mucous-secreting glands ensures lubrication and rapid immune surveillance. “This epithelium combines softness with selective strength,” notes mucosal immunologist Dr.
Raj Patel, “offering protection without sacrificing the body’s need for nuanced interaction with fluids and microbes.” Its survival hinges on constant regeneration, ensuring damage from friction or pathogens is swiftly repaired.
These two epithelial types exemplify nature’s dual strategy for protection: durability in exposed tissues and adaptability in delicate internal spaces. Their layered architecture, cell types, and biochemical uniqueness reflect evolutionary precision in balancing defense with function.
Together, keratinized and nonkeratinized stratified squamous epithelium form an invisible, yet indispensable, fortress that sustains health from the skin’s surface to the body’s innermost linings. As science deepens its understanding of these tissues, new insights emerge—ushering in potential therapies for skin disorders, wound healing innovations, and breakthroughs in mucosal immunity. The battle beneath your skin is not just a story of form—it is a testament to life’s enduring resilience.
The Evolution and Structure of Stratified Squamous Epithelium
Stratified squamous epithelium evolved as a fundamental adaptation enabling multicellular animals to survive in terrestrial and dynamic environments. Unlike simpler epithelial layers, its multi-layered design minimizes vulnerability by distributing mechanical stress across successive cells. Keratinization, a process marked by controlled proliferation and terminal differentiation, strengthens this barrier—most notably in keratinized layers exposed to abrasion.This differentiation route is tightly regulated by signaling molecules like bumpy protein and p63, which orchestrate keratin synthesis and desquamation. “Evolution optimized this system to resist wear while maintaining viability,” underscores Dr. Maria Chen, a cellular biologist studying epithelial repair.
Nonkeratinized epithelium, by contrast, reflects the necessity of permeability and sensory integration—features critical in moist tissues where exchange and responsiveness dominate over rugged defense.
Separating Structure and Function
The structural divide between keratinized and nonkeratinized layers reveals their specialized roles. In keratinized zones—such as the epidermis—cells undergo massive terminal differentiation: cell nuclei vanish, cytoplasm accumulates keratin filaments, and intercellular connections harden into a dense, cross-linked matrix.This constructs a near-impermeable shield that withstands environmental assaults for days or even years before sloughing off in a process known as desquamation. Nonkeratinized epithelium, prevalent in oral, genital, and gastrointestinal linings, retains a viable, living surface layer where basal cells continue mitotic division, replenishing the epithelium’s inner cohort. “High cell turnover allows these tissues to rapidly replace damaged cells without compromising barrier integrity,” explains Dr.
Chen. This distinction—durability versus regeneration—defines their anatomical placement and physiological significance, illustrating evolution’s trade-off between permanence and renewal.
Clinical and Functional Significance Across Tissues
The clinical implications of these epithelia extend far beyond structural definition.Keratinized stratified squamous epithelium’s role in preventing infection is unmatched; its failure manifests in conditions like eczema or psoriasis, where barrier breakdown exposes underlying tissues to irritants and microbes. Meanwhile, disruptions in nonkeratinized linings—seen in oral lichen planus or cervical dysplasia—compromise immune surveillance and moisture control, increasing susceptibility to infection and atrophy. Understanding these roles informs dermatological treatments, wound care innovations, and mucosal regenerative strategies.
The intricate coordination between protective posture and physiological responsiveness defines the battle beneath the skin. Keratinized epithelium rages silently, constructing an armor that shields from decades of external assault, while nonkeratinized tissue dances with moisture, sensation, and resilience in hidden crevices. This duality reflects evolution’s genius—crafting living tissues that are both unyielding and alive, rigid where needed, flexible where vital.
In every stratified layer, the body defends with precision and purpose, proving that protection runs not just on surface defenses, but on a complex, coordinated system written into the very fabric of our skin.



Related Post
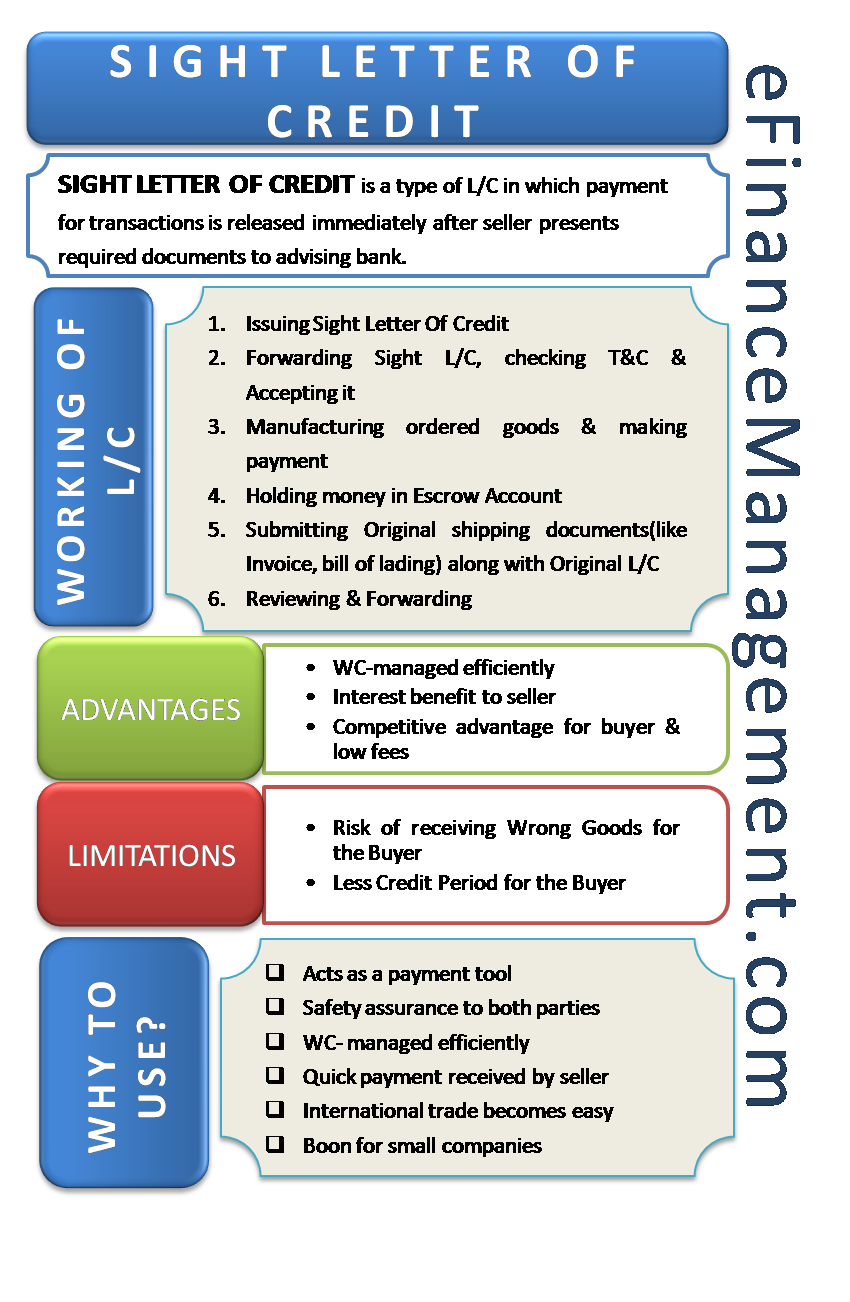
Letter Of Credit At Sight: Everything You Need to Know About This Critical Trade Finance Tool

Mario Arturo Moreno Ivanova: Architect of Cultural Diplomacy and Innovation in Arts Leadership

Charles Donald Fegert: Architect of Lutheran Phonetics and Modern Evangelical Scholarship

Tom Mison’s Family Revealed: What Media Exclusive Insights Reveal About His Roots and Legacy

